| What is cystic fibrosis? | |||
| Symptoms | |||
| Hidden issues | |||
| Useful Links |
One young man’s positivity enriches Lodge St. Patrick
Lodge St. Patrick’s meetings can never ever be said to be dull; always interesting, they are entertaining events consistently well stocked with bons amis and banter. It would also be fair to say that, as a Lodge, the members do not take themselves over seriously, but that does not infer that as a group we are blasé when it comes to concentrating our attention on guests of the calibre of one young man who attended earlier this year. His youth belying his virtually transcendent inner strength, 18-year-old Dylan Booth suffers from cystic fibrosis, a dreadfully debilitating disease that has the capability of fatally damaging many of the body’s vital organs - especially the lungs and digestive system.
Dylan (the Grandson of our Immediate Past Master, Wayne Darling) was accompanied on Lodge night by the Chairman of Cystic Fibrosis Otago, Julian Cox, a man who proved to be one of the best speakers that Lodge St. Patrick has invited in recent years. He informed us that one in 3,179 births result in a child being born with cystic fibrosis (CF), and that more than 500 people in New Zealand have the disease, of whom over 20 reside in Otago. Julian’s own daughter, Rachel Cox, sufferers from cystic fibrosis, so he was well-qualified to detail in basic terms just how invasively destructive CF is, not simply in terms of the obvious detrimental effects the disease has on the physical well-being of the person, but also the seemingly endless daily stress that the life-limiting illness inflicts on the parents, not to mention the disruption it creates within family life in general.
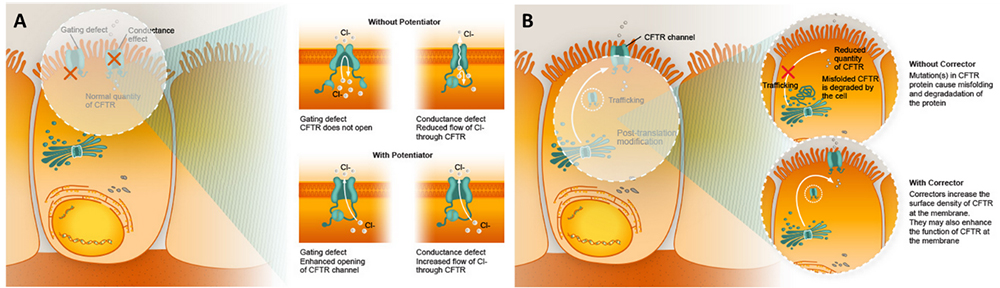
Julian told the Lodge, that cystic fibrosis is the most common, recessively-inherited, chronic and progressive disease in New Zealand, and that it is an affliction that is characterized by the excessive production of thick clogging mucus within the body. CF is caused by a defect in the CFTR (cystic fibrosis trans-membrane conductance regulator) gene, which compromises the normal function of the secretory glands. In a healthy person, mucus is a slippery and watery substance, but in CF patients it is sticky and thick – and a perfect breeding ground for bacteria.
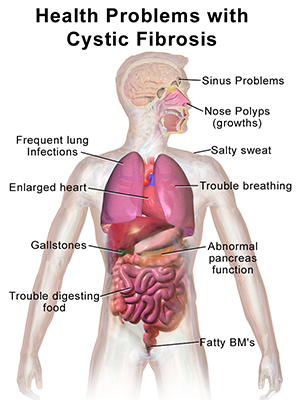
For CF sufferers in the final stages of life, Julian said that he had been told that, “It’s like drowning … one breath at a time.” It is an extremely unpleasant illness; the lungs, liver, pancreas, heart, intestines, sinuses and sex organs are the main organs affected. In the lungs, the airways become clogged; patients experience difficulty breathing and, as the thick mucus traps infection-causing bacteria, extensive lung damage and, eventually, respiratory failure results. In the pancreas, the mucus prevents the release of digestive enzymes that allow the body to break down food and absorb vital nutrients, such as fat-soluble vitamins (A, D, E and K), leading in turn to malnutrition and poor growth. The heart can become enlarged; while in the liver the bile duct can become blocked inducing liver disease. CF also causes sterility in males.

Despite the fact that there is no actual cure for cystic fibrosis, over the years progressive medical research has led to the development of a spectrum of treatments that have increased a patient’s life expectancy from less than 10-years in 1970 to almost 40 in 2017. Perhaps there is a little light at the end of a long dark tunnel.
Julian debunked one ill-informed (but quite widely held) idea that cystic fibrosis can be infectious. He explained that, being a genetically inherited disease, CF cannot be ‘caught’ by a healthy person, however, was “vital” he said, to keep individual CF patients from meeting as they can, and readily do, transmit new infections to each other. Thus it was not feasible for sufferers of the illness to share like-experiences or comfort one another face- to-face. Just another hidden cruel factor that comes as a package-deal with this killer.
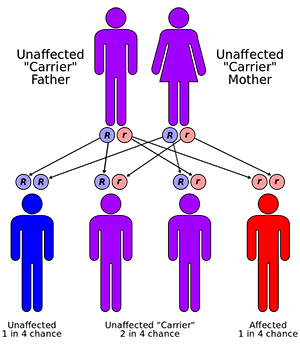
Genetics
People with CF have inherited two copies of the defective CF gene – one copy from each parent. BOTH parents must have at least one copy of the defective gene. People with one copy of the defective gene are called ‘carriers’, but do not have the disease. Each time two carriers have a child, the chances are:
25% (1 in 4) their child will have cystic fibrosis
50% (1 in 2) their child will be a carrier but will not have CF
25% (1 in 4) their child will not be a carrier and will not have CF
The defective cystic fibrosis gene contains a slight abnormality called a mutation. The difficulty in treatment lies with the fact that there are currently more than 1,700 known mutations of the disease but unfortunately most tests only screen for the most common mutations. The test results therefore may indicate that a person who IS a carrier of the CF gene is NOT a carrier. There are about 100,000 diagnosed patients in the world though, according to Dr. Preston W. Campbell of The John Hopkins Hospital in Baltimore, milder forms of the disease are often under-diagnosed with doctors believing that other illnesses such as asthma, nontuberculosis mycobacteria, aspergillosis or pancreatitis are causing the problems, when the real culprit is some level of cystic fibrosis.
Symptoms
CF sufferers can possess a variety of symptoms that include:
Very salty-tasting skin
Persistent coughing, at times with phlegm
Frequent lung infections, which include bronchitis and pneumonia
Wheezing and shortness of breath
Poor growth or weight gain in spite of having a good appetite
Difficulty with bowel movements
Infertility in males
Treatments
The type and severity of CF symptoms can differ widely from person to person and, therefore, although treatment plans can contain many of the same elements, they have to be tailored to each individual’s unique circumstances. People with CF need to work closely with their medical professionals and families to create individualized treatment plans.
Each and every day, people with cystic fibrosis are forced to complete a combination of the following therapies:
Have their airways cleared to help loosen and get rid of the thick mucus that builds up in the lungs. Some airway clearance techniques require help from family members, friends or respiratory therapists. In the U.S. many people with CF use an inflatable vest that vibrates the chest at a high frequency to help loosen and thin the mucus. The latter is a useful therapeutic device, but one that is not common in New Zealand.
Take inhaled medicines to open the airways or thin the mucus. These are liquid medicines that are made into a mist or aerosol and then inhaled through a nebulizer. These medicines include antibiotics to fight lung infections and therapies to help keep the airways clear.
Take pancreatic enzyme supplement capsules to improve the absorption of vital nutrients. These supplements are taken with every meal and most snacks. People with CF also usually take multivitamins.
One might think that a lung transplant would be the obvious cure but, as Julian explained, such complex surgery can bring with it dire complications (such as organ rejection), that can be as life threatening as CF itself and, therefore, a lung transplant is only an absolute “if all else fails” measure.

Through the Cystic Fibrosis Foundation in America, in 2015 the FDA approved a new medication to treat the root cause of cystic fibrosis, the defective protein called CFTR (SEE ABOVE). The arrival of this group of drugs, called CFTR modulators, signals a historic breakthrough in how CF is treated. It is hoped that CFTR modulators could add decades of life to some people with certain types of CF. Indeed today, there are a number of foundations, organizations and research institutes focused on developing lifesaving new therapies for ever larger numbers of people with CF. These dedicated teams pursue cutting-edge research that, no doubt one day, will develop at least a lifelong containment and probably a cure. In 1981, New Zealand became the world’s first country to introduce a national neonatal screening programme employing the ‘Guthrie heel prick test’ for seven rare but potentially serious conditions, including cystic fibrosis.
Hidden issues
Dylan’s father, Arthur Booth, described the tension that such a constantly life-threatening sickness builds up within the family. He told of the neverending back and fro trips to the hospital for therapy. He explained how what would usually be a minor ailment such as a common cold for a normal healthy person, can result in days of hospitalization for those who are afflicted with cystic fibrosis. Arthur has helped Dylan through his illness since his birth; he informed us that he often feels guilty for unknowingly ‘passing on’ the defective gene that has inflicted so much suffering, yet he also described how the illness had forced the pair to be together often. That cystic fibrosis had, in an aberrant way, caused them to “grow up together” and drawn them closer than a father and son might otherwise be in an ordinary family; “a lining of silver in the cloud,” he said.
Addressing the audience, Dylan Booth was very philosophical about his life-span reducing illness, informing us that he lived his life to the fullest extent he could manage. That he loved fishing and hunting and doing all the things young men like to do; that he was surrounded by good friends and felt that he was much better off than some other people that he had met - especially in hospital. “There are plenty of people worse off than me,” Dylan said. Later Rt.W.Bro. Professor Frank Griffin PDGM, told Dylan that it was “totally inspirational” to meet a young man who possessed such a “positive outlook” on life while struggling through such an awful illness.

The social and well-attended refectory supper was interspersed with gales of laughter, not least when Dylan’s great-uncle, Lodge Secretary, V.W.Bro. Mel Darling introduced Dylan to his first ever taste of fine Irish whisky. As Mel told us, “Judging by the look on his face, I think it might be his last!”
If this narrative were being written 40 years ago Dylan would probably not have seen his tenth birthday, yet today he could journey to 40 or 50 and well beyond as, year-on-year, medical developments extend the life expectancy of CF patients. Presently, great faith is being placed in a molecular treatment for cystic fibrosis – nanoscience at its (current) zenith. This new molecule – a protease inhibitor - is not a treatment that will simply alleviate the symptoms of this misery-making disease but, it is hoped, one that will neutralize it completely.
To a man, the members of Lodge St. Patrick are all behind such budding medical experimentation flowering into medical breakthrough - and sooner rather than later - as we have met one exceptional young man who has bravely battled cystic fibrosis for eighteen tough years and, having met him, we reckon he deserves a break.
JW-P
**NOTE:
Cystic Fibrosis Otago
Although the organization does such selfless work for CF sufferers and their families, Cystic Fibrosis Otago is entirely self-funded, relying heavily on the income from one collection day during any calendar year. Occasional donations from individuals help, and Lodge St. Patrick was pleased to contribute, but Cystic Fibrosis Otago revolves around a special bunch of caring people who deserve so much more. If you are in any position to assist them, they would be more than grateful.
Useful Links
Cystic Fibrosis Otago www.cfnz.org.nz
John Hopkins Hospital, Baltimore www.hopkinsmedicine.org
The Cystic Fibrosis Foundation (U.S.A.) www.cff.org
The American Journal of Respiratory and
Critical Care Medicine (The Blue Journal)
www.atsjournals.org